Atrial Septal Defect (ASD) can be effectively treated by transcatheter closure.

An atrial septal defect (ASD) is a hole in the wall between the two upper chambers of the heart (atria). The condition might present in newborns (congenital defects) and adults. Small defects may never manifest signs and symptoms and may be found incidentally during check-ups. In adults, signs or symptoms may begin when reaching certain age. Related signs and symptoms might include getting lung infection easily during childhood, enlarged heart, shortness of breath, tiring easily especially after activity, heart palpitations or skipped beats. If left untreated, heart palpitation might lead to fatal conditions such as heart rhythm abnormalities (arrhythmias) and heart failure presenting with peripheral gangrene which is probably too late to be successfully treated.
Being aware of warning symptoms and having regular heart check-ups remain essentially important. If atrial septal defect is detected, it can be effectively treated by transcatheter closure, a less invasive procedure with a quick recover.
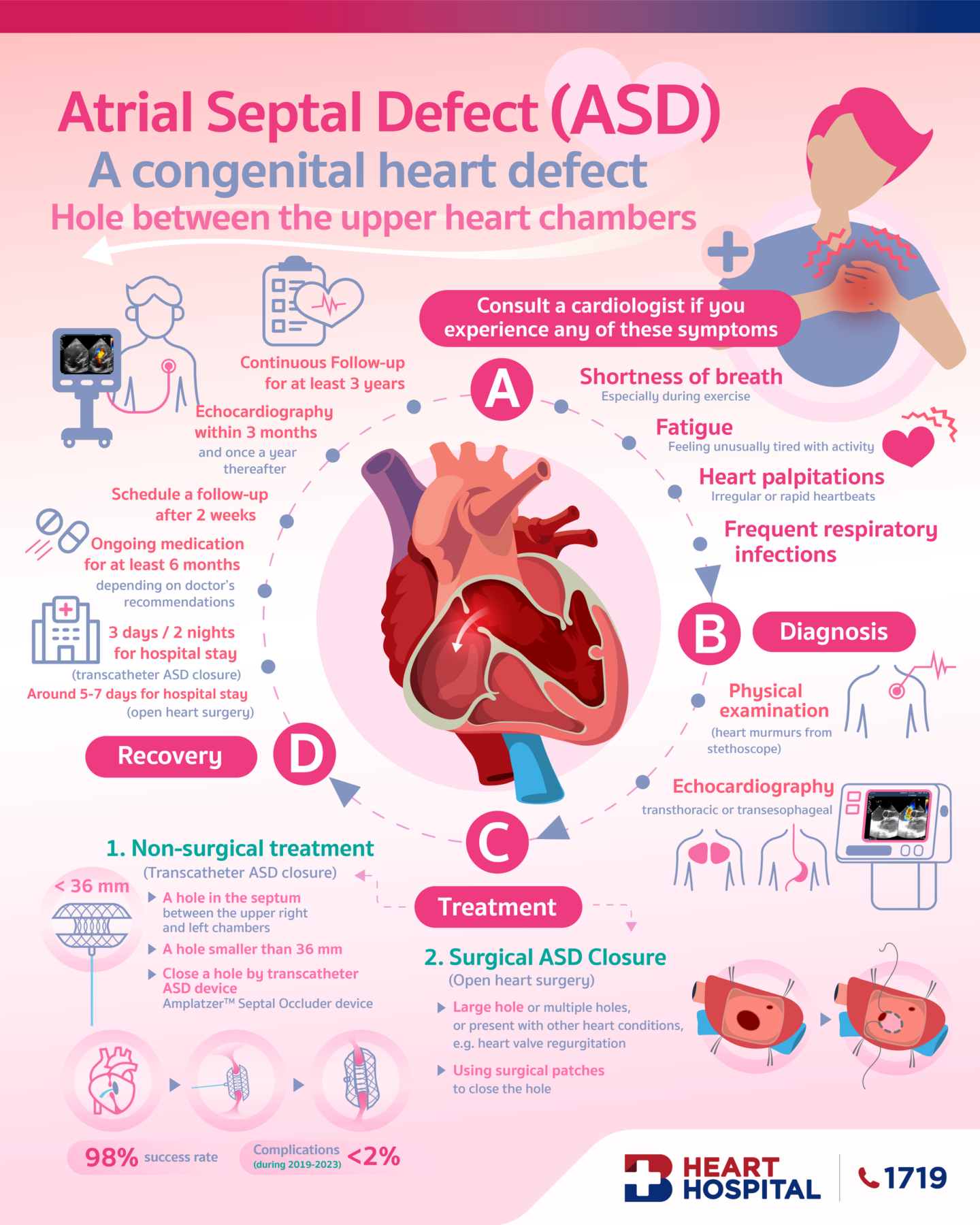
Get to know “atrial septal defect”
An atrial septal defect (ASD) is a hole in the septum which is the muscular wall that separates the heart’s two upper chambers (atria). An atrial septal defect can be a congenital defect that happens when the septum does not form properly. As a result, an atrial septal defect allows freshly oxygenated blood (received from the lung) to flow from the left upper chamber (left atrium) into the right upper chamber of the heart (right atrium). Therefore, oxygenated blood mixes with deoxygenated blood and is subsequently pumped to the lungs, even though it is already refreshed with oxygen. If the atrial septal defect is large, this extra blood volume can overfill the lungs and overwork the right side of the heart. If left treated, the right side of the heart eventually enlarges and weakens. If this process progresses, the blood pressure in the lungs may increase, leading to pulmonary hypertension.
Small defects in children may not exhibit signs and symptoms and it may be found incidentally during annual health check-ups. Predominant sign detected by cardiologists is heart murmur, a whooshing sound that can be heard through a stethoscope. Presenting symptoms might include shortness of breath, tiring easily especially after activity, heart palpitations or skipped beats. In some cases, stroke-related symptoms might be presented. Atrial septal defects can be categorized into several types. Secundum atrial septal defect is the most common type, accounts for 75% of all cases. The hole of secundum atrial septal defect occurs in the middle of the wall between the atria (atrial septum).
Diagnosis of atrial septal defect
Tests and procedures to diagnose atrial septal defect include:
- Listening to the heart using a stethoscope.
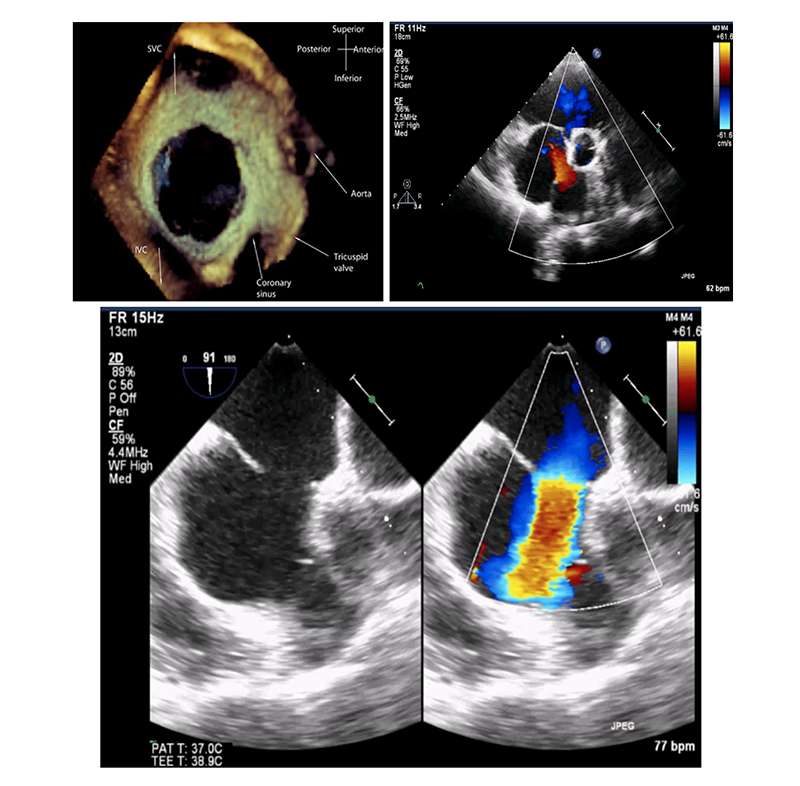
- An echocardiogram. During echocardiogram, sound waves are used to produce a video image of the heart. It allows the cardiologists to view heart’s chambers and measure their pumping strength. There are 2 common types of echocardiogram
- Transthoracic Echocardiogram: During performing this test, the probe (or ultrasonic transducer) is placed on the chest or abdomen of the patient to get various views of the heart. Although no special preparation is required, this diagnostic test might not be suitable in patients with thick chest wall or abnormal anatomy of chest wall.
- Transesophageal Echocardiogram: A specialized probe containing an ultrasound transducer at its tip is passed into the patient’s esophagus which runs behind the windpipe (trachea) and heart. Moving images of the heart can be viewed, allowing cardiologists to diagnosed accurately.
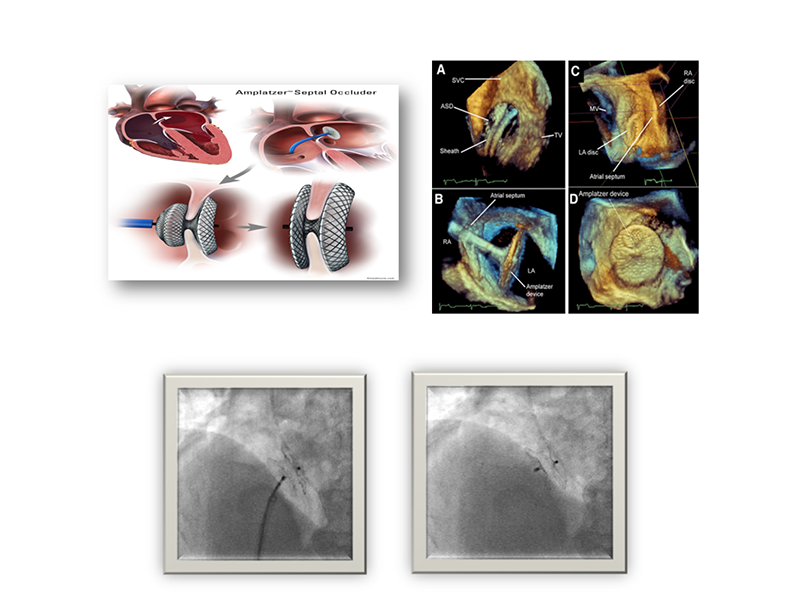
Treatment of secundum atrial septal defect
Small atrial septal defects might close on their own but it is fairly rare. If small atrial septal defects do not cause any problems, they may not require any treatment. But many persistent atrial septal defects eventually require treatments to be corrected. If the hole is larger than 1 cm. (medium sized) to 3 cm. (large sized), immediate medical attention provided by highly experienced cardiologists must be sought. Effective treatment option is “transcatheter ASD closure” which is a less invasive procedure with a quicker recovery time.
In transcathete ASD closure procedure, an interventional cardiologist inserts a thin tube (catheter) into a blood vessel in the groin and guide it to the heart using imaging techniques. Through the catheter, a mesh patch or plug is placed to close the hole. The heart tissue grows around the mesh, permanently sealing the hole within 3-6 months. Chosen material to close the holes entirely depends on the characteristic and size of the holes. In comparison with open surgery, advantages of transcatheter ASD closure include smaller incisions, less pain, fewer complications and faster recovery time within 48 hours. As a result, patients can quickly return to their daily life and activities. After receiving treatment, close follow-ups are required as scheduled, every 1, 3, 6 months and 1 year. And all medical advices given by cardiologists must be strictly followed.
To achieve the best possible outcomes derived from transcatheter ASD closure, highly experienced and trained cardiologists supported by cutting-edge technology and well-equipped catheterization room are crucially vital. In addition, transcatheter ASD closure with ASD occluder device results in high success rates with fewer complications.
Nevertheless, selected treatment option is primarily determined by size, location and type of the holes as well as individual’s conditions. Transcatheter ASD closure might not be suitable for some atrial septal defects with complicated conditions e.g. large hole (larger than 36 mm.), several holes with hole borders are smaller than 5 mm or in patients presenting with other heart diseases e.g. heart valve regurgitation. These conditions may require open-heart surgery as a first-line treatment.